| Child Kidney Dis > Volume 22(1); 2018 > Article |
|
Abstract
Ureteropelvic junction obstruction is one of the common causes of hydronephrosis in infancy and childhood. Most cases of ureteropelvic junction obstruction are diagnosed prenatally and are usually asymptomatic. Although less common, older children can experience ureteropelvic junction obstruction that presents with symptoms including flank or abdominal pain. Here, we present the case of a nine-year-old healthy girl who had repeated flank pain and abdominal symptoms, with mild left hydronephrosis, for several months. Computed tomography that was performed during the period of acute flank pain revealed aggravated hydronephrosis on her left kidney, which was secondary to an ureteropelvic junction obstruction. She underwent laparoscopic pyeloplasty, and a crossing vessel that passed the ureteropelvic junction was identified. In addition, we reviewed the current literature of this rare entity.
Ureteropelvic junction (UPJ) obstruction is a functional or anatomical obstruction of the proximal ureter that appears at the junction of the renal pelvis. Because the urine cannot be excreted from the renal pelvis into the ureter easily, excessive urine accumulates in the renal pelvis, and the collecting system slowly expands resulting in hydronephrosis [1]. UPJ obstructions, in most cases, are diagnosed by prenatal ultrasonography and are likely to have functional obstruction due to intramural defective smooth muscle or nerve development with aperistaltic segment. This kind of UPJ obstruction has no clinical symptoms except for a palpable mass and is managed during infancy.
In rare instances, children without a previous diagnosis of fetal hydronephrosis may develop UPJ obstruction at an older age because of intrinsic or extrinsic obstructive factors or both. An intrinsic stricture, polyp, and/or tumor may cause an intrinsic type of UPJ obstruction, whereas a crossing vessel, tissue band(s), fixed kinks, or angulation are likely to cause an extrinsic obstruction [2,3]. These patients usually report a medical history of periodic acute abdominal or flank pain showing spontaneous resolution. It is important to suspect UPJ obstruction in patients presenting with such symptoms and perform an ultrasonographical examination during an acute episode because ultrasonography in asymptomatic patients may show normal findings or only mild hydronephrosis and thereby delay the diagnosis of UPJ obstruction [4].
Herein, we describe the unusual case of a 9-year-old girl who presented with repeated flank pain and vomiting and in whom we found and corrected a left UPJ obstruction attributable to a crossing vessel.
A 9-year-old girl was referred to our pediatric nephrology clinic with an ultrasound finding of severe left renal hydronephrosis. She underwent renal ultrasonography for repeated vomiting, dizziness, and flank pain occurring over the last three months. Those symptoms were periodic, happening every 1 to 2 weeks, and improved spontaneously without specific treatment. When she came to our clinic, her symptoms had already disappeared. We performed renal ultrasonography, which revealed an OnenŌĆÖs grade 1 hydronephrosis on the left kidney with normal ureter. Blood and urine test results were unremarkable, and physical examination was noncontributory. Reflux was not found in the voiding cystourethrogram. At that time, we thought that her previous hydronephrosis had improved by the removal of exogenous factors such as renal stones, and we planned to observe her symptoms regularly in our clinic. Ten days later, she visited the emergency room with sudden vomiting and left flank pain. Renal ultrasonography was performed again, but the degree of hydronephrosis in her left kidney was similar to that of the last study without ureter dilatation or a visible radiopaque stone. The odd thing about her flank pain was that it seemed to improve when she vomited. Her symptoms improved spontaneously while waiting in the emergency room, and we decided to send her home.
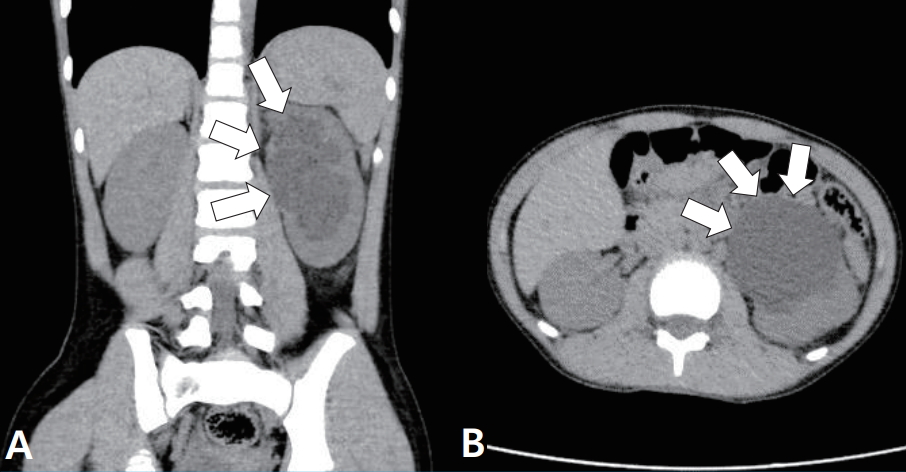
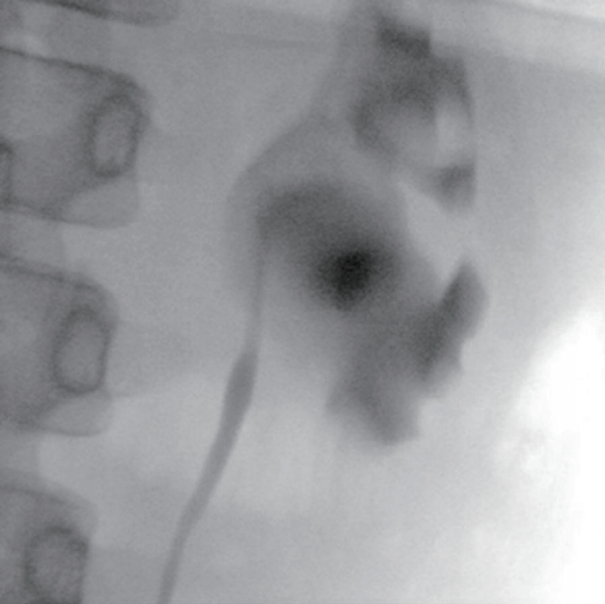
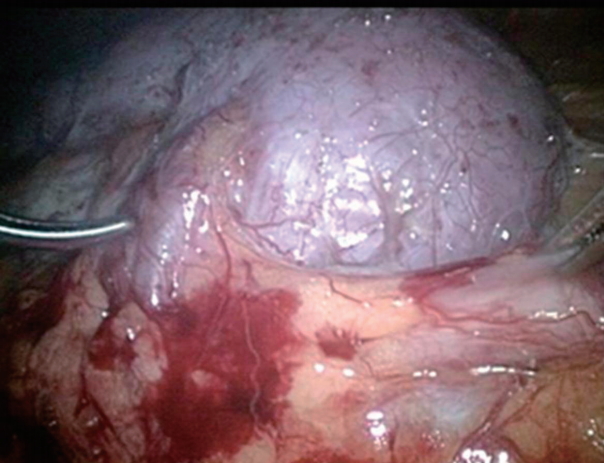
Two weeks later, she came back to the emergency room and complained about the same symptoms she had before. On physical examination, a tender mass was palpable with 2 fingers breadth at the left upper quadrant area of her abdomen. A computed tomography without contrast enhancement demonstrated the OnenŌĆÖs grade 3 hydronephrosis in her left kidney and obstruction of the left ureteropelvic junction (Fig. 1). A diuretic renal scan (Tc-99m MAG3) showed excretion from the renal collecting system after administration of the diuretic, suggesting nonobstructive hydronephrosis. Considering the possibility of extrinsic compression, a laparoscopic pyeloplasty was performed. The retrograde pyelogram demonstrated mild narrowing of the ureteropelvic junction (Fig. 2). A crossing vessel was identified passing anterior to the proximal ureter toward the lower pole of the kidney, causing extrinsic compression on the ureteral wall (Fig. 3). Some of the ureteral segment was excised, and the ureter was repositioned and anastomosed anterior to the crossing vessel. The indwelling ureteral stent was removed a month later without complication. Postoperative ultrasonography showed improvement of left hydronephrosis to OnenŌĆÖs grade 1 with a renal pelvis AP diameter of 12 mm. She has now remained symptom free for more than 16 months.
Children with symptomatic UPJ obstructions experience sudden severe episodic pain that resolves spontaneously, which occasionally is indistinguishable from benign recurrent abdominal pain observed in childhood. In most patients presenting with symptomatic UPJ obstruction, surgical correction is needed for persistent symptoms and possible renal deterioration. Therefore, it is important to raise awareness among physicians/clinicians who might have limited experience regarding this phenomenon to enable early diagnosis in these patients.
Several studies have shown that the incidence of UPJ obstruction caused by a crossing vessel is between 11% and 18.5% among all children presenting with UPJ obstruction [4,5]. However, the incidence was reported to be as high as 49ŌĆō58% for those who present later in childhood [6,7].
The symptoms of UPJ obstruction due to a crossing vessel include colicky flank or abdominal pain, nausea, vomiting, and a palpable flank mass. Renal colic has been previously reported in 30ŌĆō59% of patients with symptomatic UPJ obstruction [8,9]. These symptoms are caused by an enlarged kidney that compresses the blood vessels and other viscera. Therefore, a few patients might experience relief of these symptoms after vomiting or urination.
Ultrasonography and computed tomography at the time of symptom occurrence are essential because intermittent hydronephrosis can only be detected when the patient is symptomatic [10]. Diuretic renal scans and functional magnetic resonance urography can also provide additional information. However, there is no definitive imaging modality to accurately detect a crossing vessel causing UPJ obstruction [11].
Surgical correction is indicated when the patient is clinically symptomatic, has decreased renal function, and shows evidence of obstruction that is observed on a renal scan, and it is suspected they have crossing vessels causing these features. An open Anderson-Hynes dismembered pyeloplasty is the gold standard treatment to correct UPJ obstruction in children. Recently, laparoscopic and robotic pyeloplasty have shown outcomes similar to those of an open approach [12,13].
In conclusion, this report highlights that in older children presenting with episodic flank or abdominal pain who also show varying degrees of intermittent hydronephrosis on ultrasonographical examination, further diagnostic imaging may be warranted to accurately identify a clear etiology of the hydronephrosis and to detect a potential crossing vessel.
Acknowledgement
The authors declare that there are no potential conflict of interests regarding the publication of this paper.
References
1. Belman A.B. Ureteropelvic junction obstruction as a cause for intermittent abdominal pain in children. Pediatrics 1991;88(5):1066-9.

2. Alberti C. Congenital ureteropelvic junction obstruction: physiopathology, decoupling of tout court pelvic dilatation-obstruction semantic connection, biomarkers to predict renal damage evolution. Eur Rev Med Pharmacol Sci 2012;16(2):213-9.

3. Carter Ramires DM, Tu HY, Braga LH. Ureteropelvic Junction Obstruction by a Long Intraluminal Polyp and a Concurrent Crossing Vein in a Symptomatic 8-Year-old Child. Urology 2015;86(3):599-601.


4. Evison G. Intermittent hydronephrosis: a unique feature of ureteropelvic junction obstruction caused by a crossing renal vessel. Radiology 1986;159(1):283.

5. Rooks VJ, Lebowitz RL. Extrinsic ureteropelvic junction obstruction from a crossing renal vessel: demography and imaging. Pediatr Radiol 2001;31(2):120-4.


6. Cain MP, Rink RC, Thomas AC, Austin PF, Kaefer M, Casale AJ. Symptomatic ureteropelvic junction obstruction in children in the era of prenatal sonography-is there a higher incidence of crossing vessels? Urology 2001;57(2):338-41.


7. Rooks VJ, Lebowitz RL. Extrinsic ureteropelvic junction obstruction from a crossing renal vessel: demography and imaging. Pediatr Radiol 2001;31(2):120-4.


8. Ross JH, Kay R, Knipper NS, Steem SB. The absence of crossing vessels in association with ureteropelvic junction obstruction detected by prenatal ultrasonography. J Urol 1998;160:973-5.


9. Rigas A, Karamanolakis D, Bogdanos I, Stefanidis A, Androulakakis PA. Pelvi-ureteric junction obstruction by crossing renal vessels: clinical and imaging features. BJU Int 2003;92(1):101-3.

10. Chiarenza SF, Bleve C, Fasoli L, Battaglino F, Bucci V, Novek S, et al. Ureteropelvic junction obstruction in children by polar vessels. Is laparoscopic vascular hitching procedure a good solution? Single center experience on 35 consecutive patients. J Pediatr Surg 2016;51(2):310-4.


11. Weiss DA, Kadakia S, Kurzweil R, Srinivasan AK, Darge K, Shukla AR, et al. Detection of crossing vessels in pediatricureteropelvic junction obstruction:Clinical patterns and imaging findings. J Pediatr Urol 2015;11(4):173.e1-5.

- TOOLS
-
 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link XML Download
XML Download Full text via DOI
Full text via DOI-
 Download Citation
Download Citation
- Download Citation
-
- Close
 Print
Print-
Share :
-
METRICS

-
- 1 Crossref
- 0 Scopus
- 8,981 View
- 125 Download
- Related articles