A Case of Acute Idiopathic Scrotal Edema in a Newborn
Article information
Abstract
Acute idiopathic scrotal edema (AISE) is a self-limiting condition that is characterized by acute scrotal swelling and erythema. AISE is a very rare cause of acute scrotum, especially in neonates. We report a case of AISE in a 26-day-old infant who was admitted to the outpatient clinic with swelling and erythema of the penis and scrotum for a week. His vital signs were stable, and laboratory findings were non-specific. A diagnosis of AISE was made using scrotal ultrasonography with color Doppler. His symptoms resolved within four days after the onset of supportive treatment, and he was discharged from the hospital. In neonates with an acute scrotum, AISE should be considered to prevent unnecessary surgical exploration.
Introduction
The acute scrotum is defined as having an acute onset and is characterized by scrotal pain, swelling, and redness [1]. The most common causes of acute scrotum are testicular torsion and acute epididymo-orchitis. Acute idiopathic scrotal edema (AISE) is a cause of acute scrotum, characterized by scrotal swelling and erythema [2,3]. Ultrasonography with color flow Doppler can exclude the diagnoses of testicular torsion and acute epididymo-orchitis and can lead to the diagnosis of AISE through the identification of the fountain sign. Previous studies have shown that AISE occurs most often in patients between the ages of 5 and 11 years, but is rare in neonates [4]. Since AISE is a benign, selflimiting disease without complications, it is an important differential diagnosis to avoid unnecessary interventions or surgical exploration of the scrotum [5, 6]. This case describes a neonate diagnosed with AISE using color flow Doppler ultrasound.
Case report
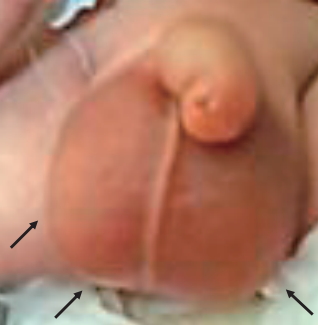
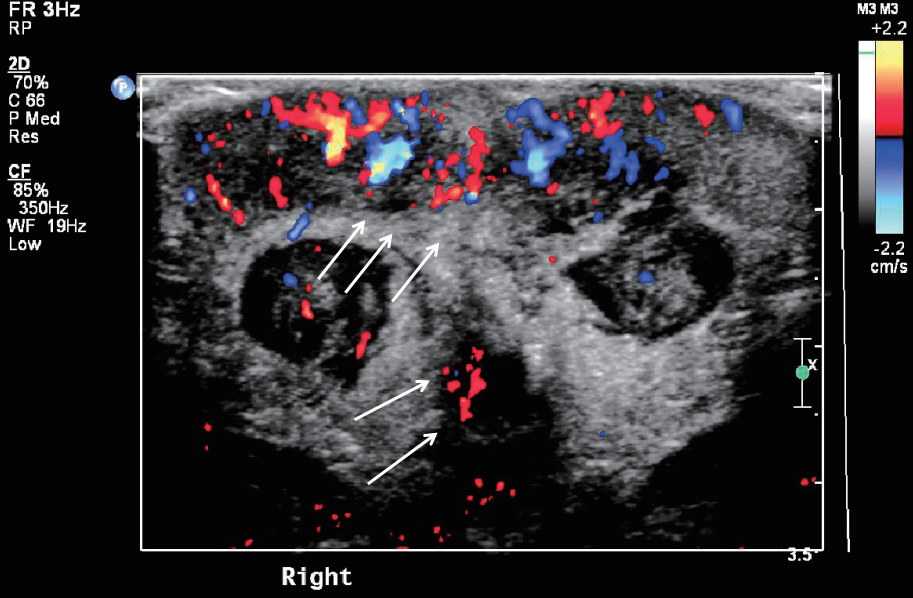
A 26-day-old baby presented to the outpatient clinic with penile and scrotal swelling and redness for a week. He was delivered at 36 weeks’ gestation in our hospital. He was born through vaginal delivery. He had a mild muscular ventricular septal defect but had no history of surgery or medication use. He had no fever or dysuria. He was 51.8 cm tall (29 percentile) and weighed 4.2 kg (31 percentile). His vital signs were normal, with a temperature of 37.1℃, heart rate of 138 beats/min, and respiratory rate of 36 breaths/min. There was no irritability or lethargy. On physical examination, he had diffuse scrotal edema and penile swelling (Fig. 1). The trans-illumination test was negative. The laboratory findings on admission were as follows: hemoglobin level, 9.9 g/dL; leukocyte count, 9,700/mm3 (neutrophils 16.9%, lymphocytes 71.9%, monocytes 8.5%, eosinophils 2%); platelet count, 294×103/mm3; aspartate aminotransferase , 26 IU/L; alanine aminotransferase level, 7 IU/L; protein, 4.5 g/dL; albumin level, 3.1 g/dL; blood nitrate urea, 3.7 mg/dL; serum creatinine, 0.1 mg/dL; erythrocyte sedimentation rate, 2 mm/hr; C-reactive protein 0.12 mg/L. His urinalysis results were normal. We performed ultrasound to differentiate the causes of acute scrotum. There was no evidence of testicular torsion or epididymitis. There were characteristic findings of AISE on ultrasonography, which showed a normal scrotum and epididymis but with the scrotal sac showing diffuse edematous swelling bilaterally. There was no ascites, lymphadenopathy, or hydrocele. Subcutaneous fat layers revealed increased vasculature on color Doppler ultrasound, with a fountain sign appearance (Fig. 2). The diagnosis of AISE was made and the patient was managed conservatively with scrotal elevation. Four days later, his symptoms improved markedly, and he was discharged from the hospital. One month later, his scrotal and penile swelling disappeared.
Discussion
AISE is one of the many causes of an acute scrotum, with symptoms such as scrotal edema and pain. In acute scrotum, 46% of cases are due to testicular torsion or torsion of the appendage, and 35% are due to acute epididymo-orchitis [7]. AISE has a prevalence of about 12–20% [2]. AISE is a pediatric disease usually seen in children younger than 10 years of age, occurring most commonly between the ages of 5 and 8 years. Of the children diagnosed with AISE, 9% are under 2 years of age, and the disease is very rare in neonates [8,9]. Here, we showed a case of AISE in a 26-day-old newborn with swelling and erythema of the penis and scrotum for a week.
Although AISE was first described by Qvist in 1956 [3], the etiology is still unclear. Allergic reactions are currently the most likely suspected cause. It is known that 40% of patients have associated asthma, eczema, and dermatitis, and eosinophilia is present in 20% of cases [10]. In addition, scrotal trauma, insect bites, urine loss to the scrotal area, and cellulitis may be causative factors. Scrotal redness and swelling are the most common clinical signs of AISE, and scrotal pain and tenderness, scrotal, penile, perineal, and inguinal area swelling are often coexistent [8]. Of the patients who are symptomatic, the majority have unilateral involvement, while bilateral involvement is seen in 1/3 of cases. In our case, the patient had edema and redness in the scrotal and inguinal areas bilaterally. However, other symptoms were not visible and any specific cause could not be found. The characteristic features of AISE are sudden onset and rapid progression, with or without the presence of fever. Laboratory studies are usually normal. Color flow Doppler ultrasound is the most important tool for diagnosing AISE. The specific ultrasound findings for AISE are edematous scrotal wall thickening, hyperemia of the scrotum, and normal appearance of the testicles. The characteristic color flow Doppler ultrasound findings include scrotal wall thickening and increased vascularity in the subcutaneous area with the appearance of water pouring from a fountain. Geiger first reported on the "fountain sign,” which is highly suggestive of AISE [4]. The fountain sign results from the markedly increased hypervascularity of the scrotal wall, which receives its blood supply from the branches of the deep external pudendal and internal pudendal arteries through the sacral arteries [4]. In a systemic review of AISE, the fountain sign showing hypervascularity was observed in 57 patients who underwent color Doppler ultrasonography [9]. We also observed the fountain appearance using color Doppler ultrasonography in our case. As the fountain sign is a characteristic feature of AISE, we made a diagnosis of AISE, although it is very unusual in neonates.
Ultrasonography can be used to differentiate between AISE, testicular torsion, epididymitis, and testicular trauma in an acute scrotum. In testicular torsion, there is hypovascularity of the affected testis. With epididymitis, there is increased vascularity with increasing size of the epididymis. Testicular trauma may present with intratesticular hematoma or laceration of the tunica albuginea. While testicular torsion should be treated surgically [2] and epididymitis should be treated with antibiotics, AISE is a benign, self-limiting condition. Unnecessary surgery or treatment can be prevented through an accurate diagnosis [11]. The treatment of AISE involves pain control and conservative management with scrotal elevation. Symptoms usually resolve within 2–4 days without complications [7]. Acute scrotal discoloration with pain upon palpation in neonates is usually caused by testicular torsion. A rare case of acute scrotum in a newborn caused by renal vein thrombosis has been shown on the first day of life [12]. In our case, a 26-day-old infant was presented with sudden scrotal and penile swelling without any other cause. Ultrasonography was performed to differentiate acute scrotum from other diseases. Ultrasonography showed no features of testicular torsion or epididymitis, but a fountain sign was found. Because the fountain sign is a characteristic feature of AISE, we made a diagnosis of AISE. With only conservative management, there was improvement of symptoms.
In conclusion, AISE is an uncommon cause of acute scrotum but important to recognize since it is a self-limiting condition. Here we report a case of AISE in a 26-day-old neonate who presented with acute scrotal and penile swelling. Although AISE is very rare in neonates, clinicians should consider AISE in a newborn with acute scrotum and perform color flow Doppler ultrasonography to distinguish it from other conditions.
Notes
Conflict of interest
No potential conflict of interest relevant to this article was reported.
Patient consent
The study was approved by the institutional review board (IRB) and the consent was waived due to the nature of the retrospective study