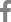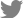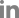A 12-year-old girl visited the ChildrenŌĆÖs Hospital in Vientiane Capital, Lao PDR with severe bony deformities and progressive paralysis of the extremity muscles. The patient was born via normal vaginal delivery without any perinatal complications. Her birth weight was 2.9 kg. She was breastfed since birth and started solid food at 6 months of age, and she completed vaccination as scheduled. She is the second child of the family, and her growth and development were normal until the age of 8 years. (
Fig. 1A) At the age of 8 years, she had a bicycle accident, resulting in dislocation of the right hip and wrist joints. After that, she was bedridden and stayed at home without treatment because of the very challenging socioeconomic status of the family. The range of motion of her upper and lower extremities gradually decreased, accompanied by progressive limb bone deformities. She also lost appetite and weight. At the age of 12 years, the patient visited the outpatient clinic at the ChildrenŌĆÖs Hospital in Vientiane Capital, Lao PDR once but only received a multivitamin prescription without an accurate diagnosis. However, her symptoms gradually worsened resulting in severe contracture of extremity joints and whole-body muscle weakness. Therefore, she visited the ChildrenŌĆÖs Hospital again.
Her father had been healthy until the age of 30 years, when he had progressive paralysis of both arms after working hard, cutting trees. After some treatment and physical therapy at a military hospital, the symptoms of the left arm improved, but the weakness in the right arm continued to this day. Her mother, sister, and cousins were healthy, without any medical condition.
At admission, her body weight was 10 kg (<3
rd percentile, she weighed 20 kg at the age of 8 years just before the bicycle accident, according to her father), and her height was 87 cm (<3
rd percentile). She was bedridden and looked cachectic. She had a rachitic rosary on the thoracic wall and severe bony deformities with tenderness in the upper and lower extremities. (
Fig. 1BŌĆō
F) A blood test showed hypokalemia (2.3ŌĆō2.8 mEq/L), metabolic acidosis (serum HCO
3ŌĆō15 mEq/L) with normal anion gap (13 mEq/L). Serum calcium level was 8.0 mg/dL, phosphorus 1.0 mmol/L, sodium 135 mEq/L, and chloride 107 mEq/L. Urine pH was high (6.6ŌĆō9.0 by dipstick) and the specific gravity was 1005. There was no proteinuria or hematuria. The urine anion gap was 78 mEq/L. Kidney ultrasonography showed normal sized kidneys with bilateral medullary nephrocalcinosis. Other laboratory tests revealed the following: WBC, 5,500; hematocrit, 38%; hemoglobin, 13 g/dL; platelet, 407,000/mm
3; serum creatinine, 0.4 mg/dL; alkaline phosphatase, 1,340 IU/L; and blood sugar, 116 mg/dL. The patient was clinically diagnosed with dRTA and was treated with oral sodium bicarbonate (started from 2.4 g/day and increased to 9.4 g/day), potassium phosphate (4 g/day), vitamin D (400 IU/day), and high calcium diet for 4 months, and then sodium bicarbonate was changed to potassium citrate (Urocitra
┬«, Pharmbio Korea, Inc., 3ŌĆō5 mEq/kg/day). Her general condition began to improve after one month of Urocitra treatment, and the follow-up laboratory tests revealed serum HCO
3ŌĆō, 21ŌĆō24 mEq/L; potassium, 4.1ŌĆō4.6 mEq/L; and phosphorus, 6ŌĆō6.5 mmol/L. She could stand alone, ride a bike, and attend school after 2 months of treatment. After 6 months of treatment, her body weight and height increased to 15 kg and 98 cm, respectively. After 2.5 years of treatment, she underwent two orthopedic surgeries for correction of the limb bone deformities in the Department of Pediatric Orthopedic Surgery, Seoul National University ChildrenŌĆÖs Hospital, Seoul, Korea with financial support from the Seoul National University ChildrenŌĆÖs Hospital Fund. Two years after the corrective surgery, plate removal from both legs was performed in the Mittaphab Hospital, Lao PDR. (
Fig. 1GŌĆō
K) Currently, she is 17 years old with a height of 133 cm and taking potassium citrate (Urocitra, 1 mEq/kg/day) only.
 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link XML Download
XML Download Full text via DOI
Full text via DOI Download Citation
Download Citation
 Print
Print