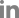Introduction
Renal cortical necrosis (RCN) is patchy or diffuse ischemic destruction of the renal cortex caused by greatly diminished renal arterial perfusion secondary to vascular spasm and microvascular injury [1]. It is a catastrophic illness with high morbidity and mortality. Obstetric complications, such as puerperal sepsis, postpartum hemorrhage, and eclampsia are the main (60% to 70%) causes of RCN in developing countries. The remaining 30% to 40% of the cases of RCN is caused by non-obstetrical causes, such as sepsis and hemolytic uremic syndrome (HUS) [1]. The incidence of RCN is higher in developing countries than in developed nations, ranging from 6% to 7% of all cases of acute kidney injury (AKI) [2,3]. RCN is very rare, especially in children, so there are few case reports of RCN in children [4]. The gold standard for the diagnosis of RCN is renal histology and RCN is classically known to progress to end-stage renal disease. Here, we review a pediatric case of RCN with AKI which showed a full recovery from AKI.
Case report
A 15-year-old boy was referred to our hospital from a local hospital due to a sharp decrease in renal function. He presented with acute back and abdominal pain, nausea with vomiting, and oliguria for the past two days. He took a single dose of antihistamine for nasal congestion and developed sudden abdominal and back pain. He had been healthy at birth, with a gestational age of 37 weeks and with a birth weight of 4,660 g. He had no history of any specific illness but his mother had type 2 diabetes. The data obtained at the local hospital showed a blood urea nitrogen (BUN) of 14 mg/dL and a creatinine (Cr) level of 1.8 mg/dL. Proteinuria (dipstick 3+) with microscopic hematuria (10ŌĆō15 red blood cells/HPF) was observed. Renal insufficiency was rapidly aggravated, showing a Cr of 2.9 mg/dL 12 hours after the first measurement. At our hospital, he had a peak blood pressure of 148/83 mmHg. He was very obese with a high body mass index (BMI) of 32.9 kg/m2 (>97 percentile). His height was 168 cm (50 percentile) and his body weight was 93 kg (>97 percentile). His vital signs were stable, except for the finding of hypertension. He appeared acutely ill, but his mental state was alert. His breath sounds were clear, and there was no cardiac murmur, hepatosplenomegaly, or generalized edema. Tenderness was found in both costovertebral angles. Laboratory findings were as follows: white blood cell (WBC) 9,120/uL, hemoglobin 12.4 g/dL, platelets 219,000/uL, C-reactive protein 1.49 mg/dL, BUN 28.4 mg/dL, Cr of 4.26 mg/dL, estimated glomerular filtration rate using Schwartz formula 16.3 ml/min/1.73m2, cholesterol 135 mg/dL, protein 8.6 g/dL, albumin 5.3 mg/dL, uric acid 9.9 mg/dL, amylase 49 U/L, and lipase 37 U/L. C3, C4, anti-double-stranded DNA antibody and anti-neutrophil cytoplasmic antibody were all normal. In urinalysis, proteinuria [spot urine protein to creatinine ratio (uPCR) 1.66)] and pyuria (5ŌĆō9 WBCs/HPF) were observed. The fractional excretion of sodium was 2.9 percent. A urine culture was sterile. Kidney sonography showed parenchymal swelling and increased renal echogenicity. AKI due to acute tubular necrosis (ATN) or acute tubulointerstitial nephritis (TIN) was initially suspected. To manage his hypertension, a continuous infusion of a calcium channel blocker (nicardipine) was administered from the first day of admission. Due to the rapidly progressive feature of nephritis affecting his renal function, steroid pulse therapy (methylprednisolone 750 mg/IV) was administered on the second day of admission and the patient recovered from his anuria and showed a complete recovery to normal renal function. The BUN was normalized to 10.4 and the Cr to 0.75 a week after his admission. His proteinuria was also reduced (uPCR 0.3) on the fifth day of admission. However, kidney biopsy findings on the second hospital day (after the steroid pulse therapy) showed renal cortical hemorrhagic necrosis. Multifocal, relatively well-circumscribed, hemorrhagic necrotic areas (about 25%) were detected in the tubulointerstitium. There were no segments of sclerosis, adhesion, or crescents. Arterioles were unremarkable (Fig. 1). Immunoreactivity for human IgG, IgA, IgM, C1q, C3, fibrin, and kappa and lambda immunoglobulin light chains were all negative. Due to the lack of suitable structures, an electron microscopic study was not performed. After discharge, the patient showed normal renal function and renal sonography revealed no pathologic findings one year later.
Discussion
Although RCN in children has virtually disappeared in high-income countries, we experienced a rare case of RCN with AKI in a 15-year-old boy. He presented with acute abdominal and back pain, nausea with vomiting, and oliguria. A sharp decrease in renal function was observed in a very short period of time. While we could not find any specific cause for the abrupt decrease in renal function, the patient was very obese. Due to the rapidly progressive course affecting his renal function, steroid pulse therapy was done and the patient completely recovered from his AKI. This work reveals the importance of early suspicion and the proper management of RCN given its poor outcome.
RCN was first described in 1886 by Juhal Renoy [4]. It accounts for about 2% of intrinsic AKIs. About two-thirds of the reported cases of RCN have been associated with pregnancy but most of the remainder occurred due to bacterial infections in non-pregnant women, males, and children [5]. The exact pathogenic mechanism of RCN is not completely known. Renal hypo-perfusion (postpartum hemorrhage) and vascular endothelial injury (HUS, eclampsia, toxin, sepsis, acute pancreatitis, and intravascular hemolysis) could be possible factors. Both renal hypo-perfusion and endothelial injury stimulate the release of endothelin from vascular endothelial cells, which causes renal damage leading to RCN [1]. Long ago, Campbell and Henderson [5] described RCN in infancy and childhood in the setting of severe dehydration, congenital heart disease, fetomaternal transfusion, perinatal asphyxia, severe hemolytic disease, and sepsis. Notably, a case of bilateral renal cortical necrosis following acute pancreatitis was recently reported in a 24-year-old male, who presented with complaints of severe upper abdominal pain and multiple episodes of vomiting for two days [6]. In our case, the patient was very obese, with a BMI of 32.9 kg/m2, however, his pancreatic enzymes were not elevated. Clinical and laboratory findings showed no evidence of sepsis, hemolysis, or severe dehydration. While he took a single dose of antihistamine, the drug did not seem to be the cause of the renal toxicity. Notably, recent studies suggest that AKI is common in obese critically ill patients and that obesity is an independent risk factor for developing AKI [7,8]. In a cohort study including 15,470 critically ill patients, the incidence and adjusted risk of AKI progressively increased with higher BMI. Each increase in BMI by 5 kg/m2 was related with a 10% risk for more severe AKI [7]. In a large Austrian study, severely obese patients had greater than 2-fold increase in severe AKI than normal weighted patients [8]. Although the pathophysiology of obesity-associated AKI is not fully understood, obesity-induced risk factors (glomerulopathy, low-grade inflammation, endothelial dysfunction, augmented oxidative stress, activation of the renin-angiotensin-aldosterone system and increased sympathetic nervous system activity), obesity-associated risk factors (metabolic syndrome, hypertension, cardiovascular disease), and other common causes (hypotension, sepsis and nephrotoxins) can precipitate AKI in critically ill obese patients [9]. A complex interplay between these different pathophysiologic mechanisms may underlie a predisposition of obese patients to more severe AKI. While we could not find any specific cause of the RCN in our patient, it is plausible that morbid obesity may have affected and/or worsened the renal impairment, leading to acute severe loss of kidney function.
The diagnosis of RCN is based either on imaging studies or histologic findings in a kidney biopsy. In light microscopy, coagulative necrosis involves all tubular segments and glomeruli and thrombi may be present in the vessels at the edge of the infarct. Diffuse or patchy necrosis is seen in electron microscopy [10]. RCN is sometimes regarded as the pathological progression of ATN which leads to cortical necrosis [1]. Although the gold standard for diagnosis is histologic findings, imaging studies help to accurately localize and identify the extent of the lesions. Kidney sonography shows enlargement of the kidneys with reduced blood flow and CT shows an absent opacification of the renal cortex with the enhancement of subcapsular and juxtamedullary areas [11]. In our case, a CT scan was not done and renal sonography showed parenchymal swelling and increased renal echogenicity. The process of diagnosis was difficult and finally, the patient was diagnosed with an incomplete form of RCN through the renal histologic findings. Since the kidney biopsy was performed after steroid pulse therapy, the renal pathology might have been partially affected by the steroid administration.
The aim of the management of RCN is to maintain hemodynamic stability and treat the underlying diseases. Hemodialysis should be started early to prevent metabolic disorders and blood pressure should also be controlled to stop the progression of further kidney damage [12]. There have been no studies on steroids as therapeutic options for RCN but rapidly-administered steroid therapy is known to be an important treatment for acute TIN assisting in the recovery of renal function [13]. Because steroids attenuate the inflammatory response after the induction of AKI and alleviate renal dysfunction [14], steroid pulse therapy may have positively affected the recovery of renal function in our patient. Unlike our case, a recent report noted that steroid therapy showed no response in the case of a 21-year-old woman and that the patient required renal replacement therapy with hemofiltration. The patient did not recover renal function and remained on regular dialysis [15]. Further research is needed to evaluate the effects of steroids in the acute phase of RCN. Irreversible loss of kidney function is the most natural course of complete cortical necrosis but the prognosis varies in the incomplete type, where less than 50% of the nephrons are necrotic [16]. Patients with incomplete necrosis can experience restoration of their kidney function, depending or the extent of renal involvement [6]. In our case, the prognosis was good because our patient showed an incomplete type of RCN where the hemorrhagic necrotic areas were about 25% in the tubulointerstitium of the biopsy specimen.
Taken together, we report a 15-year-old boy with RCN who showed a complete clinical recovery of his AKI. Although RCN is an unusual cause of AKI in children, pediatricians should consider the possibility of RCN when evaluating patients with rapidly decreasing renal function, especially in severely obese children. Suspicion is very important in the RCN diagnosis because it is difficult to diagnosis RCN before a kidney biopsy. Because of the catastrophic sequelae of RCN, early diagnosis and aggressive management should be undertaken for better renal outcome and prognosis of the patient.



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print